
Executive Dysfunction in Adults
Executive Dysfunction in Adults:
More Than Just Procrastination
At our practice in Mooresville, Concord, and Denver, NC many adults share stresses around their own self management and follow through. While most people have put off a task at some point, these people are concerned about never following through. A phone call goes unreturned, laundry sits in the basket for days, or an important email remains unfinished even though you have read it three times. From the outside, it can look like procrastination. From the inside, it can feel much more complicated.
Many adults live with executive dysfunction without realizing it. They may describe themselves as scattered, unmotivated, or overwhelmed – when in reality the issue may involve the brain’s ability to manage and organize daily life.
Executive functioning refers to the mental skills that help us plan, focus, remember, regulate emotions, and complete tasks. When those skills are not working efficiently, even simple responsibilities can begin to feel exhausting.
What Executive Dysfunction Can Look Like in Adults
Executive dysfunction can show up in ways that are easy to dismiss as personality traits or bad habits. Adults will experience difficulty starting tasks even when they want to do them or chronic procrastination. Difficulties with keeping up with appointments, deadlines, or managing time expended on tasks is also a common complaint. If you think of yourself as “being a mess” because of constantly losing things like your keys or personal items – this too could be executive dysfunction.
Even those you would think of as a high performer may still struggle with executive functioning. When you have experienced a moment of being mentally frozen due to overwhelm, or even just have experienced general overwhelm in the face of multiple responsibilities – you have experienced a struggle in executive functioning.
Someone may appear capable in one area of life while quietly struggling in another.
A person can be highly intelligent and still find it difficult to consistently manage everyday demands.
Why It Is Often Misunderstood
Executive dysfunction is frequently mistaken for laziness. Adults who struggle with it often hear that they need to try harder, or that they need to be more organized and disciplined. From an outside perspective people will say everyone procrastinates, but internally that is not the case.
The problem is that executive dysfunction is not simply about knowing what to do. Often, the person already knows exactly what needs attention. The challenge is translating intention into action.
This misunderstanding can create and lead to shame. Many adults begin to believe something is wrong with their character instead of recognizing that there may be a deeper issue affecting their functioning.
What Can Contribute to Executive Dysfunction

Several factors can contribute to executive dysfunction, such as:
- ADHD
- Anxiety
- Depression
- Chronic stress
- Trauma
- Burnout
- Sleep deprivation
Stress in particular can make executive functioning worse. When our nervous system stays in survival mode, our brain has less energy to focus on planning, organizing, and self-regulation.
How It Impacts Daily Life
Executive dysfunction can affect almost every aspect of life. This can include missed deadlines or incomplete projects at work. At home executive dysfunction can turn into unfinished chores, forgotten errands, or difficulty maintaining a routine. In our relationships, partners or family members may misinterpret your struggles as carelessness or a lack of effort. Self-care can decline as well by forgetting medications, eating irregularly, or not getting enough sleep.
Many adults describe feeling like they are constantly behind, no matter how hard they are trying.
The Emotional Toll
One of the most difficult parts of executive dysfunction is the emotional impact that comes with it.
Adults may feel:
- Frustrated with themselves
- Embarrassed by their struggles
- Ashamed that things feel harder than they “should”
- Anxious about falling behind
- Exhausted from constantly trying to catch up
Because these struggles are often invisible, many people suffer quietly. They may look successful on the outside while feeling overwhelmed internally.
Strategies That Can Help
Executive dysfunction can improve with the right support and practical tools.
Helpful strategies may include breaking up tasks into smaller steps. For example, instead of telling yourself to “clean the kitchen” you can separate tasks such as unloading the dishwasher, next wipe counters, and lastly take out the trash. Breaking up these steps can help to reduce the overwhelming feelings that may come with large tasks.
Using external systems can help to rely less on memory. These systems can include adding important events to your calendars, creating phone reminders for day to day tasks, visual checklists to break up large tasks, and setting timers.
Creating a familiar routine each day can reduce decision fatigue.
Reducing distractions can often make it easier to begin a task.
Some people can benefit from body doubling, where they focus better when there is another person nearby, even if that person is simply working quietly.
Seeking Support – Adult Therapy in Mooresville, Concord, Denver, NC
If executive dysfunction is interfering with your daily life, professional support can help.
Therapy may help identify:
- underlying anxiety
- trauma
- burnout
- attention concerns
- emotional regulation difficulties
With support, adults can begin to understand their patterns, reduce shame, and build unique strategies that actually work in their lives.
Connect with a Therapist
Moving Forward
Many adults in Concord, Denver, and Mooresville, NC seek therapy after years of believing they simply need to be more disciplined, when executive dysfunction may actually be contributing to the struggle. Executive dysfunction is often far more than procrastination. It can be a real challenge that affects how a person manages life, responsibilities, and stress.
Understanding the difference matters.
Because when people stop asking,
“Why can’t I just do this?” and begin asking, “What is getting in the way?”
Real change can begin.
Learn More

5 Signs Your Child may be Struggling After Trauma
5 Signs Your Child May Be Struggling After a Traumatic Experience
Many children experience difficult or frightening events at some point in their lives. While some children recover with time and support, others may continue to struggle emotionally or behaviorally. Trauma can affect how a child feels, thinks, and interacts with the world around them.
Recognizing the signs early can help parents get the right support and help their child begin to heal.
What Is Childhood Trauma?
Childhood trauma is events, big or small, that the child experienced as a threat to themselves or to someone they care for. What matters is the child’s experience. Even when events may not appear to be as concerning to adults, while they could have left a frightening impression on a child. For example, a child witnessed the loss of someone they are close to can be traumatic, even if the loss was expected. Other events that could be classified as trauma include witnessing any level of violence, serious accidents, medical procedures, and physical abuse or domestic violence.
Every child processes experiences differently. As noted previously, small or brief moments that went unnoted to an adult could leave a negative and lasting traumatic impact on your child. Below we are going to give you 5 signs your child may be struggling after a trauma.
5 Signs a Child May Be Struggling After Trauma
1. Changes in Mood or Behavior
Children who are struggling with the effects of trauma may act very differently than they did before those impacting events. When you see any of the following symptoms – take note.
- Increased irritability or anger
- Withdrawal from family or friends
- Loss of interest in activities they once enjoyed
- Increased clinginess or separation anxiety
2. Sleep Problems or Nightmares
Trauma can affect a child’s sense of safety, which is often revealed at bedtime. If there has been a sudden shift in night time comforting by your child, or a change in their comfortability in sleeping over at relatives or friend’s homes this could be an indicator for concern.
Sleep struggles can be any of the following:
- Difficulty falling asleep
- Frequent nightmares
- Fear of sleeping alone
- Nighttime anxiety
3. Increased Anxiety or Fear
Children who have experienced trauma may become more alert to possible dangers. This is a part of the fight or flight response that we see in any person who has gone through a traumatic event. Their neurological system can shift into high gear in order to prevent being hurt again, causing a surge in anxious feelings and behaviors.
Examples of this can include:
- Jumpiness or being easily startled
- Worrying about something bad happening
- Avoiding certain places or situations
- Strong reactions to reminders of the event
4. Trouble Concentrating at School
Trauma affects attention and memory due to the brain shifting into a survival mode for self protection. Specifically, the amygdala becomes hyperactive while the hippocampus is suppressed. This ultimately suppresses the parts of the brain that support executive functioning and rational thought.
Your child may begin showing the following shifts:
- Difficulty focusing
- Declining grades
- Trouble completing assignments
- Increased frustration with schoolwork
5. Physical Complaints Without Clear Medical Cause
In many cases, children express emotional distress through physical symptoms. This is due in part to having limited emotional vocabulary or recognition of the impacts that the environment has on them.
These health complaints can include:
- Stomachaches
- Headaches
- Fatigue
- Feeling sick before school or certain activities
When Should Parents Seek Support?
Research shows that treatment is most effective when provided as soon as possible after the event occurs. Consider seeking professional help if:
- Symptoms last longer than a few weeks
- Behaviors are getting worse instead of better
- Your child seems overwhelmed by emotions
- Daily functioning at home or school is affected
Connect with a Therapist
Trauma Therapy for Children in Denver, Concord, and Mooresville, NC
Providing care and treatment for children who have been exposed and are struggling to process traumatic events is crucial to improving their life outcomes. When treatment is not provided, long lasting emotional and behavioral health struggles can persist. There are multiple approaches for children’s treatment that are geared towards their developmental needs.
Treatment approaches include
- Trauma Focused Cognitive Behavioral Therapy (TFCBT)
- Play and Art Therapy
- EMDR
- Cognitive Processing Therapy
If your child has experienced a traumatic event and continues to struggle, it’s important to know that you don’t have to navigate this alone—support is available. With the right care, children can begin to make sense of what they’ve been through in a safe and supportive environment. Trauma-focused therapy helps children process difficult experiences, build healthy coping skills, and regain a sense of safety and stability. Over time, this support can empower them to move forward with greater confidence, resilience, and hope for the future.
Learn More

The Impact of Chronic Invalidation on the Nervous System
The Impact of Chronic Invalidation on the Nervous System
Chronic Stress, Trauma, and Healing Support in
Concord, Denver, and Mooresville, NC
When Being Unseen Becomes a Stress Response
At Miracles Counseling Centers, we often work with individuals and teens in Concord, Denver, and Mooresville, NC who feel confused about why their bodies react so strongly to relational stress. Often, chronic invalidation is part of that story.
Chronic invalidation is a form of emotional dismissal. It can come in the form of family members who minimize your feelings with phrases such as “It’s not that bad.” Or “We all go through it.” Alternatively, responses that shift blame with statements such as “Why are you so emotional” also suggest fault and invalidation of a person’s experience. These types of responses can suggest to the individuals that their feelings are wrong, irrational, or unimportant. In this article, we want to build understanding on how the brain receives and adapts to messages from the relationships you are in.
How Chronic Invalidation Affects the Nervous System
When we experience stress — especially relational stress like criticism, rejection, or chronic invalidation — our nervous system automatically shifts into protection mode. This is called the fight, flight, fawn trauma response. The brain is constantly learning, adapting, and protecting the self. In this case, it is learning that what you say you are feeling is not ok and acceptable. Let’s dig a little deeper into the types of trauma responses there are.
The 3 Trauma Responses
- The fight response shows up as defensiveness, irritability, anger, or a strong urge to argue or prove yourself. The nervous system is preparing to confront the threat.
- The flight response looks like anxiety, overthinking, restlessness, or the urge to escape the situation altogether. This can also show up as perfectionism or staying constantly busy to avoid emotional discomfort.
- The fawn response is less talked about but very common in chronically invalidating environments. Fawning involves people-pleasing, minimizing your own needs, or automatically agreeing in order to maintain safety and connection. The nervous system learns that compliance reduces conflict.
Trauma Responses are Natural
These responses are not personality flaws. They are adaptive survival strategies wired into the body. Relational stress in the form of chronic emotional suppression is not only felt, but is biologically impactful. When someone experiences chronic invalidation, the nervous system may begin to perceive everyday relational tension as a threat. In turn, activating these protective patterns even when there is no immediate danger.
only felt, but is biologically impactful. When someone experiences chronic invalidation, the nervous system may begin to perceive everyday relational tension as a threat. In turn, activating these protective patterns even when there is no immediate danger.
What is important to recognize is that the pattern of invalidation in adulthood is slow and insidious to our mental health. Childhood invalidation can be worse in some cases as it is a slow burn trauma that can last into adulthood. The impact of this builds overtime causing broad impacts to a person’s felt state to change as well as to their relationships. While a trauma response is natural, repeated exposure to trauma changes the nervous system.
What do Normal Trauma Reactions Look Like?
A few real life examples of nervous system changes could be teenagers who are described as being over reactive or moody may actually be in a response pattern, requiring teen trauma therapy work to support a nervous system that is in dysregulation. Another example are adults who are overly anxious in their lives. These adults could have been brought up in a continuously invalidating environment needing anxiety counseling to address self doubt and low self esteem.
Working with a trauma-informed therapist in Concord, Denver, or Mooresville, NC can help individuals understand these patterns, their origin, and begin restoring nervous system balance.
Long-Term Effects on Mental Health and Relationships
 Over time, repeated exposure to emotional invalidation can have significant consequences. As noted previously, these include poor self esteem and confidence, self doubt and shame, as well as anxiety and depression. Imagine moving through life, never quite fully trusting yourself. From whether you are good enough, to being able to believe you are deserving…the impact of chronic invalidation can change a person’s self perspective.
Over time, repeated exposure to emotional invalidation can have significant consequences. As noted previously, these include poor self esteem and confidence, self doubt and shame, as well as anxiety and depression. Imagine moving through life, never quite fully trusting yourself. From whether you are good enough, to being able to believe you are deserving…the impact of chronic invalidation can change a person’s self perspective.
Ultimately, chronic invalidation can change your life’s choices and outcomes. Emotional dysregulation can result in moments of extreme outbursts, or conversely, apathy and detachment and will impact your relationships. In providing depression counseling, we see these themes of emotional suppression in someone’s life story, and recognize this as a focal point in trauma treatment for healing.
Confidence and identity issues that result from emotional invalidation do affect self esteem as well. If a person has low self esteem the chances are high that they may also have poor boundaries in their relationships. Potentially, they may not feel safe to vocalize their opinions or needs, and thus remain in unsatisfying relationships that feel empty. Becoming a passive partner in a relationship is not satisfying for either individual and leaves the potential for relationship unhappiness.
Another common consequence will be a tendency towards people pleasing behaviors or on the flip side hyper-independence. Hyper-independence, is not empowerment. It is a trauma response rooted in fear. It is the response of a nervous system that learned early on that no one is coming, support will disappear, people can’t be trusted, help may not arrive, and that abandonment is a real possibility.
If relationship issues are a part of what you are struggling with, your therapist will want to learn about the messages you have received in childhood in regards to the validity of your emotions and how you have learned to express them (or not).
Healing the Nervous System: Support Is Available Locally
The nervous system can change. Even if chronic invalidation has shaped how your body responds to stress, those patterns are not permanent.
Healing begins with safety.
When someone experiences consistent emotional attunement — being listened to, believed, and responded to with care — the nervous system gradually shifts out of survival mode. Validation is not simply “being nice.” It is a biological signal of safety. Over time, that safety allows the body to reduce hypervigilance, soften shutdown patterns, and rebuild internal trust.
Trauma-informed therapy supports this process intentionally. Approaches such as Trauma-Focused Cognitive Behavioral Therapy (TF-CBT), attachment-informed therapy, and nervous-system-based interventions such as EMDR help individuals understand their stress responses and gently retrain regulation patterns. Rather than forcing change, therapy works with the body’s protective instincts while creating new experiences of stability and connection.
Small practices outside of therapy can also support regulation:
- Learning to notice body cues without judgment
- Grounding exercises that anchor you in the present moment
- Setting boundaries that reduce repeated invalidating interactions
- Building relationships where your emotions are respected
Connect with a Therapist
Trauma-Informed Therapy in Concord, Denver, and Mooresville, NC
If you or your teen notice anxiety, emotional shu tdown, people-pleasing patterns, or difficulty trusting your own feelings, support is available. At Miracles Counseling Centers, we provide trauma-informed therapy in Concord, Denver, and Mooresville, NC, helping children, teens, and adults restore nervous system balance and rebuild self-trust.
Being heard is not a luxury. It is part of how the nervous system heals.
Learn More

TF-CBT Helps Children and Teens Heal After Trauma
How TF-CBT Helps Children and Teens Heal After Trauma
Why Trauma Doesn’t Just “Go Away”
The unfortunate truth is children and teens experience trauma. The unpredictability of life will bring experiences that can cause a traumatic impact. Actually, as we have addressed in other articles, a traumatic impact does not have to necessarily be a big event. Trauma can be moments in which create emotional distress that the person doesn’t yet have the tools to process. They matter not because of how dramatic the moment was — but because of how alone, unsafe, or powerless the person felt at the time. TF-CBT for children and teens helps trauma to resolve and move out of their bodies and mind.
When children have a significant shift in their moods and behaviors, trauma potentially can underlie it. This would not be a temporary change, but a longer term shift in how they typically behave. Things that will be noted are:
- Emotional outbursts or shutdown
- Anxiety, sleep issues, regression
- Behavior changes or school struggles
The truth is, your child may not just “moody” or going through a phase. Trauma impacts the nervous system, not just thoughts. It is possible that the change your seeing is rooted in a trauma response, and Trauma Focused Cognitive Behavioral Therapy for children and teens can help.
What Is TF-CBT? (In Plain Language)
Trauma-Focused Cognitive Behavioral Therapy, often called TF-CBT, is an evidence-based approach created specifically to help children and adolescents heal after traumatic experiences. It is one of the most researched and trusted trauma treatments for young people.
At its core, TF-CBT helps kids and teens make sense of what happened to them—without overwhelming them—and learn skills to feel safe again in their bodies, emotions, and relationships.
Trauma can change how a child’s brain and nervous system respond to the world. Specificly, while a dangerous event may be over the body may still react as if the threat is present. TF-CBT for teens and children works by gently helping the brain and body relearn that safety is possible.
Who TF-CBT Is Designed For
TF-CBT is used with:
- Children and teens who have experienced trauma
- Caregivers who want to support their child’s healing
- Families who want structure, guidance, and hope—not endless therapy
It is commonly used for trauma related to:
- Abuse or neglect
- Sudden loss or grief
- Medical procedures or hospitalizations
- Accidents or injuries
- Witnessing violence or frightening events
What Makes TF-CBT Different
Unlike general talk therapy, TF-CBT is:
- Structured – there is a clear roadmap for treatment
- Time-limited – progress is intentional and goal-focused
- Developmentally appropriate – therapy is tailored to the child’s age
- Caregiver-involved – parents or caregivers are an active part of the process
This approach recognizes that children heal best when the adults in their lives understand trauma and know how to respond with consistency, safety, and connection.
A Child-Centered, Pace-Respecting Approach
One common concern parents have is whether trauma therapy will force their child to relive painful memories. TF-CBT for children and teens does not rush this process. Children move at a pace that feels manageable, and skills are built first to help them regulate emotions and feel grounded. Primarily, the goal is not to erase the memory, but to help the child understand it without fear, shame, or self-blame.
In the next section, we’ll explore how TF-CBT works step-by-step and what families can expect during the therapy process.
How TF-CBT Actually Works
In using this approach, your TF-CBT therapist focuses on three core goals:
Helping kids feel safe in their bodies again
Making sense of what happened without shame
Strengthening the caregiver-child relationship
The PRACTICE Model
The PRACTICE model is the structure used in TF-CBT to guide treatment. It helps children and caregivers build coping skills, process traumatic experiences at a safe pace, and strengthen their relationship. The steps focus on education, emotional regulation, understanding thoughts and feelings, gently processing the trauma story, and creating a sense of safety moving forward. The Practice model addresses the following 8 areas:
- Psychoeducation
- Relaxation skills
- Affective expression
- Cognitive coping
- Trauma narrative
- In-vivo mastery
- Conjoint sessions
- Enhancing safety
Parents & Caregivers are an important part!
 TF-CBT is not just individual child and teen therapy. As a result, recognizing the vital role a child’s environment and support team play in mental health, this therapy intentionally incorporates caregivers.
TF-CBT is not just individual child and teen therapy. As a result, recognizing the vital role a child’s environment and support team play in mental health, this therapy intentionally incorporates caregivers.
As a caregiver you will learn to:
→How trauma shows up behaviorally
→Ways to respond without escalating
→How to support healing at home
The importance of empowering parents with tools to support the healing at home is fundamental to recovery.
At Miracles Counseling Centers, our therapists provide Trauma-Focused Cognitive Behavioral Therapy (TF-CBT) for children and teens in
Concord, NC, Mooresville, NC, and Denver, NC.
We support young people who are ready to heal from trauma and build emotional resilience—so they can move forward with confidence, safety, and hope.
Connect with a Therapist
What TF-CBT Is Not
Trauma effects on children and teens is already difficult enough. The great part of TF-CBT for children and teens is that it is not about forcing children to relive their trauma. Nor do we want them to have to reopen any wounds without professional support offered. We will be helping children and teens not ignore their emotions, while also keeping therapy focused and time constrained. TF-CBT is structured and time focused, meaning you will not have to be involved in endless therapy that does not end.
What Progress Often Looks Like
As you and your child moves through treatment using TF-CBT you will notice that they will have less emotional dysregulation. Meaning outbursts, meltdowns, and reactivity will decrease. Ultimately, there will also be fewer reactions to trauma reminders. Overall, they will increase in confidence and sense of safety. Your home and relationship with your child/teen will feel better adjusted and have improved communication that is productive and connective. Each person is unique, and so your child and teen’s improvement will vary based upon their unique life experiences and developmental stages.
Healing is Possible with TFCBT
Healing is possible. The brain has an incredible capacity to change, and evidence-based approaches like Trauma-Focused Cognitive Behavioral Therapy for children and teens support the natural ability to heal. This work helps children and teens process their experiences from the inside out, creating meaningful and lasting change. In conclusion, young people who have lived through trauma deserve more than just coping—they deserve the freedom to grow, dream, and move forward without their past continuing to shape their future.
Learn More
When “I’m Fine” Is a Habit: How Emotional Suppression Impacts Mood Over Time
“I’m fine” is a phrase we all have used at least once or twice….maybe hundreds of times. Sometimes this is true. We can manage the situation, handle it and keep moving forward. Other times, this phrase is a way to emotionally suppress the mood we are in. Some emotions are just too hard to face at the moment. It can also feel as if it is a form of weakness if we acknowledge a negative emotion we are experiencing. Ignoring or shutting down our emotions is a learned survival skill that works, but can be overused. Those emotions we suppress don’t simply disappear – they can show up as mood shifts, irritability, or numbness and exhaustion.
What Emotional Suppression Really Is (And What It Isn’t)
Emotional Suppression vs Emotional Regulation
Emotional Suppression is the act of pushing down our emotions in order to keep functioning. The idea here is by focusing efforts you need to take to succeed or accomplish the task at hand, the better off you are. There is an idea that if you were to feel what you are going through, those feelings get in the way. Ultimately inhibiting the task at hand. This is a primary belief that leads to emotional suppression in adults.
Emotional Regulation is the act of noticing, tolerating, and processing your emotions as you experience them. The idea here is to make space in your mind for the emotions you are experiencing. Unfortunately, most adults are not taught how to use regulation skills or even have an idea that there are skills to manage emotions.
Why Emotional Suppression Feels Like Strength (At First)
The Short-Term Benefits That Become Long-Term Problems
Common reasons people believe that suppressing their emotions is needed often comes out of a sense of self preservation. It could be the need to stay productive in their job or lives. Another reason is to maintain an identity of being the “strong one” or being the “easy going” personality. Suppressing your emotions can also seen as needed so as to get through a crisis situation. Momentary use of stuffing emotions can be useful, but when it comes a lifestyle approach it can become harmful.
How Suppressed Emotions Affect Mood Over Time
The Emotional Cost of Always Being ‘Okay’
When emotional suppression is used chronically it can lead to unintended, negative consequences. A few of these include feeling emotionally numb, difficulty with mood swings or irritability and anger outbursts, and a general sense of disconnection from self or others. This is what us in the therapy world would call ‘mood disturbances’ and are often occurring repeatedly over the course of time.
The Link Between Suppression and Mood Disorders
Feeling “fine” can also lead to a belief that “nothing is wrong with me,” even when things internally feel unstable. Eventually, suppressing emotions can lead towards more persistent mood disorders such as depression, anxiety, or Bipolar Disorders. The mind can only suppressive emotions for so long until the accumulation leads to something bigger. For those who are high functioning adults, a diagnosis of depression or anxiety can be missed due to overperforming and external self management of your emotions.
Why Talking Yourself Out of Feelings Doesn’t Work
Why Logic Alone Can’t Fix Emotional Patterns
The experiences we have and the emotions they invoke do not pass through us and fade away once we move on. Feelings live in the nervous system, and create neuorpathways in our brain. This wiring slowly adjusts how we respond to our environment. From our personal relationships, to the workplace impacts will be noticed in how you respond to others or manage workload requirements. The suppression you use will eventually create an emotional pressure that has to release, in one way or another. Eventually, neurological system finds a release.
How Therapy Helps You Feel Without Falling Apart
Therapy as Emotional Relearning, Not Emotional Dumping
Participating in therapy is a learning process more so than just a conversation with a supportive person. You will learn how to be emotionally aware of your experiences, and reconnect to your authentic identity. Goals may include how to stabilize your moods, learn how to recognize emotions, and/or also build a plan for emotional tolerance of those experiences you have been avoiding. Focus on:
At Miracles Counseling Centers, our therapists support adults in Concord, Mooresville, and Denver, NC who are ready to move beyond emotional survival and into emotional stability.
Connect with a Therapist
When to Consider Reaching Out
Signs It Might Be Time to Talk to Someone
If you are in a place where you don’t know what’s wrong and just don’t feel like yourself, it may be time to connect with a therapist. Read the list below – if any of this sounds like you, then it’s time to speak with someone.
- “I feel flat, but not sad”
- “I’m functioning, but disconnected”
- “My mood feels unpredictable”
- “I’ve been strong for a long time”
Our hope in reading this is that it can be a lesson if not needed now, but possibly in the future. Our lives take many twists and turns, and this information can be insight and understanding needed for a future road you will take. Therapy can be a process of relief and support needed when suppression has taken over. Remember, that a crisis event or emotional spiraling does not need to happen before you receive the support from an objective professional. When you are ready, we are here to help provide therapy for mood regulation support in Concord, Mooresville, or Denver, NC.
Learn More

Mood Tracking for Better Emotional Health
Mood Tracking for Better Emotional Health
Why Mood Tracking Matters
When working on understanding and gaining better control of your mental health, mood tracking is a fundamental technique often recommended by therapists. Even if you are not actively involved in therapy, mood tracking can still benefit you! If you are concerned you may have a mood disorder such as anxiety, depression, or Bipolar Disorders, mood tracking can help you to see patterns over time. This can bring you clarity, reduce self-blame, and support the progress you are attempting to achieve.
If you are struggling with mood swings, energy or appetite changes, or just feeling “off” and not sure why this topic is for you! This article is going to bring light to what mood tracking actually looks like. I will also go over the specifics of what you should be noting, and why it’s an approach that will help you.
What Mood Tracking Looks Like
Mood tracking is simply an observation of your emotions. You will notate what preceded those moods, and how they impacted your thoughts and actions. Think of it as traveling back in your memories and noting what you went through recently. The goal of mood tracking is to notice patterns over time in your emotional self.
There are numerous ways to monitor your moods. Some therapists have their own logs they will assign you. If you are not in counseling right now, there are also published journals or apps to download. Sometimes a simple spiral bound notebook is all that is needed to free-write what you are experiencing emotionally. There truly is no right way to go about it, what matters is that you spend time noticing your emotional self daily so you can learn more about yourself.
Mood tracking is most beneficial when you do it consistently. Set up a time of day that works best for you, and that might help you in some way. As an example, if you tend to struggle with anxiety or motivation in the early part of your day, a morning practice of mood tracking would be good for you.
What to Pay Attention To
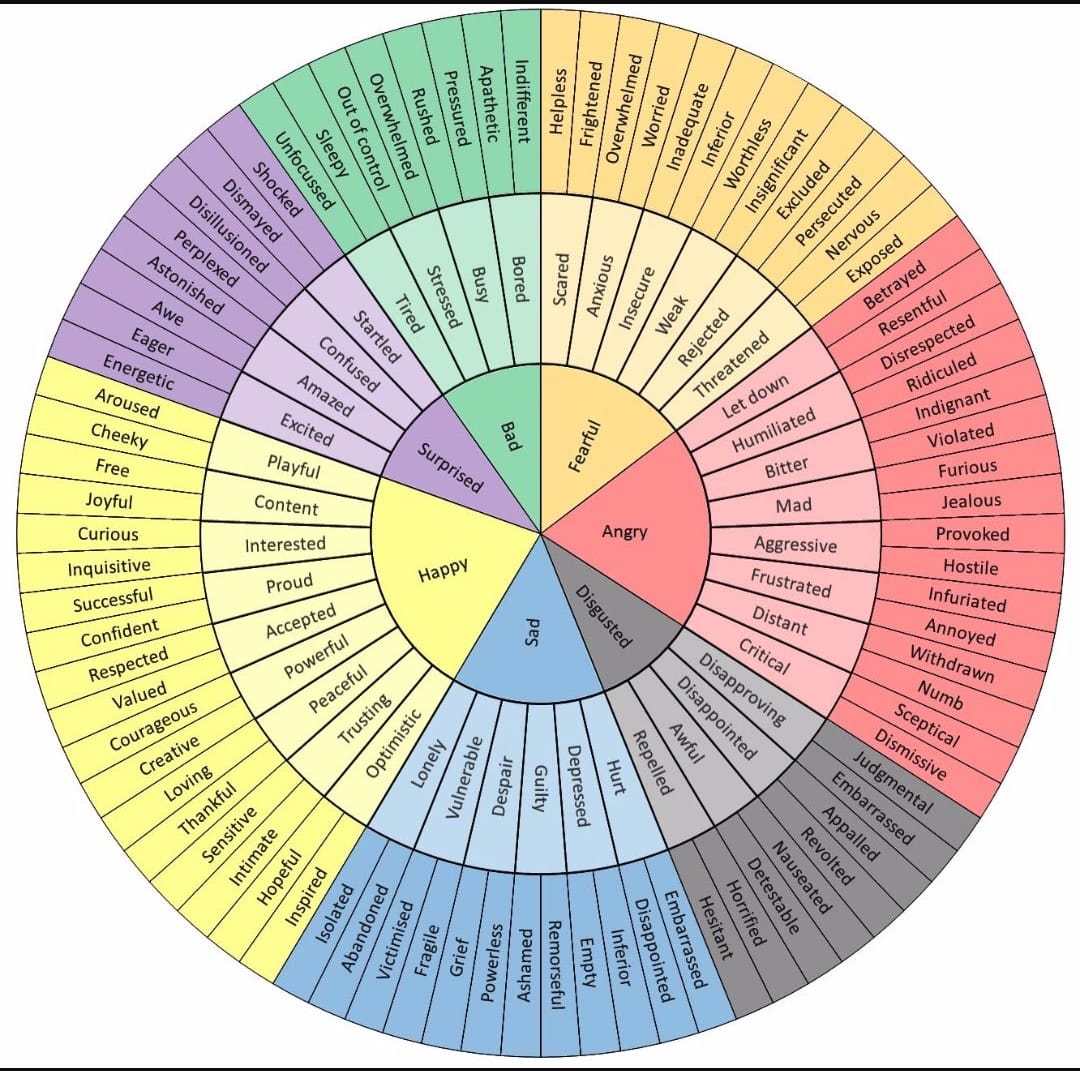
Paying attention to what moods you are experiencing is the first step to mood tracking. Depression, anxiety, stress, and anger are all feeling examples that could be monitored in your mood tracker. If you have a hard time identifying your emotions, the feelings wheel below can help you to find the words for what you are experiencing.
It’s useful to note how strong the feelings are, as well as the duration they last for. Notate what led up to those emotions, and if you attempted to cope with a negative emotion. Did that work well, or not really? Other things that you could log include your sleep, energy levels, stressors, and routines—keeping it simple so tracking feels supportive, not overwhelming.
Another interesting way to build insight is to not only do a daily mood log, but to also do a weekly reflection. This will give you even greater information into you and how you interact in the world.
I would suggest a daily and weekly reflection that takes no more than 10 minutes so as it is sustainable in your daily life. Remember, mental health practices in your life are meant to build you up, not take away from you.
How Mood Tracking Supports Mental Health & Therapy
When done consistently, mood tracking will build self-awareness.The practice of mood tracking will also help you to build the inner voice that helps you to recognize your needs in the moment. This will encourage better use of self care, coping skills, and boundaries. Even better, mood trackers provide excellent information for your therapist to help them provide you with individualized care. So whether you are seeking help for depression, or other mood disorders, mood tracking is a great step to take.
It’s important to note that mood tracking should not be used as a diagnostic tool. This is a method that should bring gentle awareness to your emotions. If you are concerned about a trend in your mood log, it would be best to review your mood log, in addition to your personal history with a clinical therapist before drawing any conclusions from your tracking.
When Tracking Signals It’s Time for Support
If you have been journaling, and mood tracking for some time you may notice a pattern by now. Are you seeing you have a persistently depressed mood? Is there a pattern of irritability and anger outbursts in your life? When mood tracking is raising more questions than answers, this is a sign that you could benefit from additional support. The work you have observing and tracking your moods up to this point will be a great jumping off point in therapy sessions.
Our therapists at Miracles Counseling Centers are all skilled at supporting your journey in reflection and ultimately building emotional balance in your life. Don’t let the work you have done up to this point slip away. Continue building upon this with one of our therapists, click the button below to begin scheduling!
Learn More

5 signs of Depression
5 signs You are Experiencing Depression
It’s understandable to experience highs and lows in life. After all, any and all emotions are a normal human experience. For example, we are sad after losing someone in our life. It’s normal to expect to be disappointed in ourselves when we receive a poor review at work. Depression is more than a temporary experience though.. It is something that can take hold of how someone feels about themselves, how they perform in the world, and change their energy levels, and ability to participate in activities.
It’s incredibly important to recognize the signs that you are experiencing depression so that you can receive the support needed to receive meaningful support and healing. Below we will go through 5 signs that you are experiencing depression.
Sign 1: Persistent Low Mood or Emotional Numbness
When we say persistent, what we mean is a low mood or numbness that lasts consistently for 2 weeks or longer. Your emotions will be sad, empty, or you are feel “flatlined” for most of the day. Things that would normally bring you excitement no longer do, and life seems to have no interest any longer. If you are experiencing this, it is a strong sign you may be struggling with a depressive episode.
It can be normal to experience this level of sadness if you have recently went through a significant loss. Following the grief process, your emotions should rise. If they do not, this could be a sign of persistent grief and should be evaluated by a therapist.
Sign 2: Loss of Interest or Pleasure
If you’ve lost your drive for the day you typically feel you could be depressed. Those who once truly enjoyed their job and looked forward to the challenge, no longer feel this way – possibly calling in sick repeatedly for no reason just to avoid the task. Or your previously enjoyed weekend activity now feels lackluster, and so you start not showing up leaving friends wondering what happened to you. As you slowly start disconnecting from people and things, your world begins to quietly shrink.
Sign 3: Changes in Energy, Sleep, or Appetite
Oftentimes, our clients who are depressed describe waking up and sensing little energy even after a full night’s rest. Other physical signs of depression are a decrease or increase in appetite and possibly a change in sleeping too much or even insomnia. Your body can feel “as heavy as rocks.” Depression can feel like chronic fatigue in anything that you do. Due to the lowering of neurochemicals released by the brain, most will experience some type of physical change when you are depressed.
Sign 4: Negative Thought Patterns
Depression changes our outlook on the world, often causing an increase in self criticism and internal thoughts of worthlessness. Depressed individuals may become negative and critical about those their lives, and may become argumentative or avoidant of others.
When you are depressed, it is possible to struggle with ruminations as well. What this means is that for an elongated amount of time you are trapped in a circular thought pattern that does not end. A person could ruminate throughout the day on the same thing, also interrupting their productivity and focus. Ruminations can be dangerous because they often will simply reinforce the negative beliefs of the depression.
Sign 5: Difficulty Functioning in Daily Life
As you can imagine when you are experiencing any or all of the above, life can be tough when you are dealing with depression. In making decisions, your focus and concentration will be impacted. Additionally due to low energy and motivation you could also be getting negative feedback at work or school on your performance. The stress of these circumstances can cause further difficulty due to the potential to react poorly towards others in irritability.
Why Therapy when your depressed helps
Therapists do more than just talk and support you when your depressed. We are the ones who are going to help you identify poor patterns of thought that are keeping you depressed. Additionally, we will help you to build a tailored plan that will work for you to build back your investment and happiness in your life. Depression is very treatable when you are engaged with the right providers. Counseling is great place to begin that can naturally and holistically help.
If you see yourself in the above, we encourage you to seek out help. The saying that “there is no better time than the present” rings true with this. Sometimes it just takes a little support to make a big change in your life.
Learn More
The Post-Holiday Slump: Your Mental Health
The Post-Holiday Slump: Your Mental Health
As the holidays come to an end, many people notice an unexpected shift in their mood. The decorations come down, routines resume, and the emotional intensity of the season fades—often leaving behind feelings of sadness, fatigue, or lack of motivation. This experience is commonly known as the post-holiday slump, and it affects people of all ages and backgrounds.
While the post-holiday slump is common, it can feel isolating if you don’t understand why it’s happening or how to respond. The good news is that with awareness, support, and intentional care, this transition period can be managed in a healthy and compassionate way.
What Is the Post-Holiday Slump?
The post-holiday slump refers to a temporary decline in mental and emotional well-being following the holiday season. Unlike clinical depression, it is typically short-term, but that doesn’t make it insignificant. Many individuals in the Lake Norman and Cabarrus County areas report feeling “off” in January and early February without knowing exactly why.
Common symptoms of the post-holiday slump include:
- Low mood or emotional flatness
- Increased anxiety or irritability
- Fatigue or lack of motivation
- Difficulty concentrating
- Changes in sleep or appetite
For some, these feelings resolve naturally. For others—especially those already managing stress, anxiety, or grief—they can linger and intensify.
Why the Post-Holiday Slump Happens
There are several reasons the post-holiday slump is so prevalent, particularly in busy communities like Mooresville, Concord, and Denver, NC, where families juggle work, school, and caregiving responsibilities.
work, school, and caregiving responsibilities.
Loss of Anticipation and Routine
The holidays provide structure, excitement, and something to look forward to. Once that ends, daily life can feel monotonous or empty by comparison.
Emotional Aftereffects
The holidays often bring up complicated emotions—family dynamics, grief over loss, financial stress, or loneliness. When the distractions end, those feelings may surface more clearly.
Burnout and Exhaustion
Travel, social obligations, end-of-year deadlines, and caregiving demands often leave people physically and emotionally drained going into the new year.
Seasonal Factors
Shorter days, less sunlight, and colder weather in North Carolina can also impact mood and energy levels, compounding the emotional slump.
How the Post-Holiday Slump Affects Mental Health
The post-holiday slump can impact both emotional and physical well-being. You may notice:
- Increased stress or anxiety returning after time off
- Difficulty re-engaging with work or school
- Feeling disconnected from others
- Questioning motivation, purpose, or direction
For individuals already receiving therapy or considering counseling in Mooresville, Concord, or Denver, this season often brings increased awareness of unmet emotional needs.
Healthy Ways to Cope With the Post-Holiday Slump
Supporting your mental health during this transition doesn’t require drastic change. Small, consistent steps can make a meaningful difference.
Normalize Your Experience
First, remind yourself that what you’re feeling is common. Emotional shifts after major life events—or seasons—are part of being human.
Rebuild Gentle Structure
Rather than forcing productivity, focus on creating simple routines: regular meals, consistent sleep, brief movement, or quiet moments to reset your nervous system.
Stay Connected
Connection is a powerful protective factor for mental health. Reach out to a trusted friend, family member, or therapist instead of isolating when motivation feels low.
Set Realistic Expectations
January does not have to be a “fresh start” or a complete reinvention. Healing and motivation often return gradually, not all at once.
Seek Professional Mental Health Support
If feelings of sadness, anxiety, or emotional numbness persist for several weeks or begin interfering with daily life, counseling can provide support, clarity, and coping tools.
When the Post-Holiday Slump Signals Something More
Sometimes the post-holiday slump is more than just a temporary dip. It may indicate underlying concerns such as:
- Depression or anxiety
- Unresolved grief or loss
- Chronic stress or burnout
- Difficulty with life transitions
Mental health counseling provides a safe, supportive space to explore these patterns and develop strategies that promote long-term emotional wellness.
Mental Health Counseling in Mooresville, Concord, and Denver, NC
Local mental health support matters. Working with a therapist who understands the pace, stressors, and community dynamics of Mooresville, Concord, and Denver, NC can help you feel seen and supported during difficult seasons.
Therapy can help you:
- Process post-holiday emotions
- Manage anxiety or low mood
- Rebuild motivation and balance
- Strengthen coping skills
- Improve emotional connection and self-awareness
You don’t have to wait until things feel overwhelming to seek help—early support often leads to more effective outcomes.
Moving Forward With Compassion
The post-holiday slump can feel discouraging, but it doesn’t define you or your year ahead. With patience, connection, and the right mental health support, this season can become an opportunity for reflection, grounding, and renewed emotional stability.
If you’re struggling during the post-holiday season in Mooresville, Concord, or Denver, North Carolina, reaching out for counseling support can be a meaningful step toward feeling more like yourself again.
Learn More

Helping Children Heal Through Storytelling
Helping Children Heal Through Storytelling
Why narrative work is one of the most powerful tools in child therapy.
Children don’t often come out and say, “I’m struggling with anxiety,” or “I think my self-esteem is low.” Instead, they say things like, “My tummy hurts,” “I don’t want to go,” or may even just start crying.
For many kids, especially those dealing with big feelings, behavior issues, sensory overload, or experiences they don’t fully understand yet, words don’t flow easily. But stories? Stories meet them exactly where they are.
Storytelling serves as a gentle, trauma-informed, creativity-based technique to help children process emotions, rebuild confidence, and develop healthier coping skills.
Let’s take a look at how storytelling works, why it’s so effective, and how parents can use the same strategies at home.
Why Storytelling Works for the Developing Brain
Kids naturally think in images, metaphors, characters, and pretend play. Their brains are wired for narratives. Ultimately, when therapists introduce stories, they’re doing more than entertaining, they’re helping a child translate emotional experiences into something their mind can understand and safely explore.
Storytelling helps children:
- Name emotions they couldn’t identify before
- Build emotional regulation skills
- Understand cause and effect
- Increase confidence and self-esteem
- Feel empowered rather than ashamed or “bad”
- Create a sense of meaning and coherence
- Strengthen communication skills
For children healing from anxiety, bullying, grief, family changes, trauma, or simply trying to navigate everyday stress, the story becomes a safe container. Basically, it gives shape to something that once felt overwhelming.
1. Using Characters as Emotional Mirrors
One of the most powerful techniques therapists use is creating or choosing characters who represent what the child is experiencing.
A child who feels angry might meet “The Volcano Dragon.”
Children with separation anxiety might hear a story about “The Little Panda Who Found Brave.”
The child who struggles with perfectionism might learn from “The Paintbrush Who Made Mistakes.”
These characters do two things at once…one, they validate the child’s inner world “Someone else feels this way too” and two they create emotional distance, a sense of “This isn’t about me, it’s about the character”. That small amount of distance is crucial. It lets kids talk openly without the pressure of direct self-disclosure.
2. Rewriting the Story to Build Coping Skills
Once the child connects with the character, therapists invite them to help “rewrite” the character’s story.
The character might learn:
- Breathing techniques “The dragon cooled his fire with slow belly breaths”
- Mindfulness tools “Koala pressed her hand to her heart when she felt scared”
- Problem-solving skills “The brave paintbrush asked a friend for help”
- Anger management strategies “The volcano found a safe place to let steam out”
- Healthy communication “The turtle learned to use his words instead of hiding in his shell”
In therapeutic language, this is called externalization shifting, where we shift from “I am the problem” to “I am someone learning skills.” For kids who struggle with meltdowns, shutdowns, anxiety, aggression, or impulse control, this small shift can be life-changing.
If we’re being honest story telling adds the “now you’re speaking my language” component to child therapy.

3. Giving Children the Role of Hero, Helper, or Wise Guide
Therapists often allow the child to take an empowered role in the storytelling process. The child becomes:
- The hero who helps the character
- The guide who offers wisdom
- The friend who understands
- The protector who keeps others safe
This is especially powerful for children who have felt helpless, scared, or overwhelmed. By helping the character, they are indirectly learning how to help themselves.
This step restores control, competence, and confidence.
4. Using Storytelling to Process Trauma Safely
For children who have gone through painful experiences, medical procedures, bullying, family conflict, loss, or other trauma… storytelling becomes a gentle entry point. Instead of recounting the event directly (which may be dysregulating or retraumatizing), the child creates a fictional scenario that mirrors the emotional experience.
This gives them a chance to:
- Make sense of what happened
- Release shame
- Explore fears
- See themselves as strong and capable
- Integrate the experience into their story instead of being defined by it
This is trauma-informed narrative work that is respectful, safe, and child-centered.
How Parents Can Use Storytelling at Home
Has reading this felt like “Wow, I can see exactly how that approach would be beneficial for my child.” You don’t have to be a therapist to use storytelling as a healing tool.
Parents can use the same techniques in daily life:
Start with a simple opening:
“Once upon a time, there was a kid who felt …”
Introduce a character who mirrors your child’s struggle:
A turtle with big feelings, a bunny with worry thoughts, a robot who needs recharging.
Give the character strengths and helpers:
Friends, wise guides, or tools that represent coping skills.
End with hope and growth never perfection:
The character doesn’t have to “fix” everything, just grow a little.
This builds safety, curiosity, and trust. Children feel seen without feeling exposed.
We’re here to help…
As you can see, storytelling is more than a creative exercise, it’s a therapeutic bridge. It helps children put language to their emotions, build healthier coping skills, and understand themselves with more compassion.
Whether used in play therapy, child counseling, or simple bedtime conversations at home, stories help children heal by giving them exactly what they need: safety, connection, imagination, and hope. If your child is navigating anxiety, behavioral challenges, low self-esteem, grief, or simply the everyday struggles of growing up, we’re here to help!
One of the greatest strengths is the ability to make meaning of our experiences… and storytelling gives children a safe way to do exactly that.
Learn More

Supporting Children after a Shooting
Supporting Children After Witnessing a Public Shooting
A Trauma-Informed Guide for Parents
When a family experiences a terrifying event like a public shooting, even if everyone makes it out physically unharmed, the emotional impact can be profound. Children may struggle to make sense of what they saw and heard, and parents are often left wondering how to help their children feel safe again. The good news is that there are clear, trauma–informed strategies that can guide families through the weeks that follow. Children are resilient, especially when their caregivers know how to support them through fear, confusion, and lingering anxiety.
First, Reestablish Safety

One of the most important things caregivers can do in the immediate aftermath is to re–establish a sense of safety and predictability. After a frightening event, a child’s nervous system can remain stuck in “alert mode,” scanning the environment for danger. Parents can help by offering direct reassurance such as, “We’re home, we’re safe, and the danger is over.” Keeping routines stable—bedtime, meals, school—also helps the body and brain settle. Limiting exposure to news footage, online videos, or an abundance of adult conversations about the incident prevents the child from reliving the trauma indirectly.
As children begin processing the event, they may or may not want to talk about what happened. Parents should allow conversations to unfold naturally rather than pushing for details. When children do speak, caregivers can validate their feelings with simple, calm statements like, “That was scary,” or “It makes sense you feel nervous.” Explanations should be brief, honest, and age-appropriate. Avoid minimizing the experience or offering analytical, probability-based reassurance—children need emotional safety dmore than statistics.
Many parents are surprised by the responses that follow trauma, but most reactions are temporary and normal. Nightmares, difficulty sleeping, clinginess, irritability, and repetitive questions are common as the brain tries to integrate a frightening experience. Children often want to revisit the event repeatedly as a way to understand it. Parents can gently reassure children that these reactions are typical and tend to improve with time. The goal is to normalize without heightening fear—“Your brain is trying to make sense of what happened. These reactions usually get better over time.”
Connection is Key

Connection plays a powerful role in helping children recover. Following a traumatic event, many kids benefit from being physically close to their parents—extra cuddles, staying in the same room at night, or sitting near the caregiver during playtime. This closeness supports co-regulation, where the adult’s calm presence helps soothethe child’s nervous system. Slow breathing together, using sensory grounding objects, and speaking in a steady, gentle tone are small actions that can have a big impact. Children take emotional cues from the adults around them; a regulated parent helps create a regulated child.
In addition to emotional connection, children need a simple, coherent narrative about what happened. A clear story anchors their understanding and reduces confusion. Parents might say, “We heard loud noises that were dangerous. We ran to get safe. The police took care of the situation, and now we’re home and safe.” It can also be empowering to highlight the protective steps everyone took—running away, following directions, staying together, or calling for help. This reinforces a sense of competence and self-trust instead of helplessness.
Practical Steps that Work
Coping tools are another valuable piece of recovery. Children respond well to grounding and sensory activities that settle the body. Naming five things they see, four they can touch, three they can hear, two they can smell, and one they can taste is a highly effective grounding exercise. Deep belly breathing, guided imagery, drawing, or expressive play are all healthy ways for kids to work through feelings that may be difficult to verbalize.
Because nightmares are common in the weeks following trauma, maintaining a predictable and soothing nighttime routine can be helpful. Children may be more likely to share their worries at bedtime. A dim nightlight, a comfort item, or a guided meditation that invites children to imagine “hanging their worries on the worry tree” before bed can help ease the transition to sleep. Some children may need a parent to stay close by until their sense of nighttime safety returns.
As families begin re-engaging with normal life, it’s essential not to force children back into crowded or chaotic environments too quickly. Healing takes time, and each child’s pace may be different. Exposure to triggering environments should be gradual and child-led. Pressuring them to “get over it” can increase fear rather than reduce it.
Recognizing When Help is Needed
While many reactions resolve on their own, parents should remain attentive to signs that additional support may be needed. Seek professional help if you observe:
- Persistent nightmares beyond several weeks
- Growing anxiety or panic symptoms
- Avoidance of school, public areas, or age-appropriate separation
- Significant sleep disruptions or regression
- Aggression, irritability, or emotional withdrawal
- Hypervigilance, such as constant scanning of the environment
These signs may indicate that acute stress is shifting toward PTSD and warrant support from a trauma-trained clinician.
If you observe the symptoms above, professional resources can make a tremendous difference. Therapists trained in TF-CBT, EMDR for children, or play therapy use structured approaches specifically designed to help young people recover from trauma, and Miracles Counseling is proud to offer all of the above. Early intervention can prevent long-term symptoms and support a healthier emotional trajectory.
You too, Deserve Support
Last, but certainly not least, it’s probably the most important thing for parents to care for themselves. Your emotional stability directly influences your child’s recovery.Acknowledge your own fear or distress, seek support from friends or professionals, and allow yourself to process the experience without burdening your child with adult-level worries. Children don’t need perfect parents, but they do need steady ones. When caregivers model healthy coping behaviors, they create the safest possible environment for healing.
Recovering from a traumatic event takes time, but children can and do heal remarkably well when surrounded by calm, supportive, and emotionally attuned caregivers. With patience, connection, and the right tools, families can move forward together with strength and resilience.
 Marisa Grimmius, LCMHCA is a trauma informed clinician, trained in EMDR. She is passionate about providing clinical care to our community, especially those who have struggled with distressing experiences. Marisa provides clinical support to adolescents 12 years and up, and adults who have life experiences that have affected them, consequently creating the subsequent symptoms of anxiety, OCD, depression, and interpersonal difficulties. She is highly knowledgeable regarding neurodivergency and autism diagnoses as well. Marisa works out of our Mooresville, NC office and is available for in person as well as telehealth therapy sessions.
Marisa Grimmius, LCMHCA is a trauma informed clinician, trained in EMDR. She is passionate about providing clinical care to our community, especially those who have struggled with distressing experiences. Marisa provides clinical support to adolescents 12 years and up, and adults who have life experiences that have affected them, consequently creating the subsequent symptoms of anxiety, OCD, depression, and interpersonal difficulties. She is highly knowledgeable regarding neurodivergency and autism diagnoses as well. Marisa works out of our Mooresville, NC office and is available for in person as well as telehealth therapy sessions.
Learn More

